Bone Graft
Bone is living tissue. At any one time, our body is forming new bone and removing existing bone in a constant process of bone remodeling. Our jawbones are strengthened by a physical stimulus such as the biting and chewing forces transmitted through the teeth. When we lose our teeth, the physical stimulus is lost over the affected area, bone is resorbed and shrinkage occurs. Bone loss may also occur due to systemic conditions such as osteoporosis.

When would I need a bone graft?
If there is severe shrinkage of the jaw bone, you may need a bone graft to regenerate bone thickness for successful dental implant placement or to provide support for dentures.
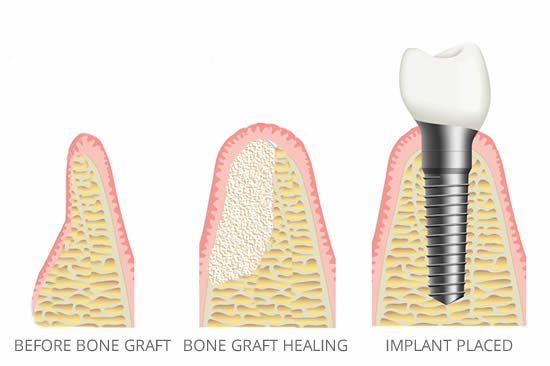
A cone-beam CT (CBCT) is usually done for the assessment of bone quality. This scan will allow the dentist to accurately measure the height, width, and density of your existing bone. If assessed to be necessary, bone grafting is offered, usually as an adjunct to implant surgery. This procedure may also be performed after dental extraction in order to preserve the site. This can be timed either at the same visit or subsequently if there are conditions such as infection limiting the integration of the grafted bone.
Bone grafting is a minor surgical procedure where the dentist prepares and secures the grafting material onto your jaw bone. It is usually performed under local anesthesia. Bone graft materials can be obtained from a few sources including the patient’s own bone from a different part of the body or most commonly, a special sterilized bone scaffolding derived from bovine sources.
 Bone loss on lower jaw (gums opened to expose bone before grafting surgery)
Bone loss on lower jaw (gums opened to expose bone before grafting surgery) Bone graft on lower jaw
Bone graft on lower jaw Regenerative collagen membrane placed between the gums and bone graft
Regenerative collagen membrane placed between the gums and bone graft
How long will it take for a bone graft to become strong and hard?
Typically, you have to wait several months for the newly-introduced bone to fuse with your jaw bone, creating strong, solid bone. A successful bone graft allows your jaw bone to be strong enough to support your dental implant, ensuring that the implant stays stable and secure.
Make an Appointment
Dental Implants
A dental implant (tooth implant) is a small titanium fixture that serves as a replacement for the root portion of a missing natural tooth. Titanium is used because it is most bio-compatible with our human body. The dental implant is surgically placed in the jawbone and functions as an anchor for the replacement tooth. After bonding takes place between the jawbone and the dental implant, the implant can provide a firm base to support a crown, bridge or denture.
Dental implants may be used to replace a single missing tooth, several teeth or a complete and functional set of dentures for individuals who have lost several or all of their teeth. Dentures and bridges mounted to implants are fitted securely and do not shift about in the mouth, a prerequisite for eating and speaking. As such, most patients report feeling more natural, secure and confident with dental implants compared to when they were using conventional dentures.
This procedure allows one or more teeth to be replaced without affecting neighboring teeth. It is thus recommended as a long-term solution for missing teeth.
 Implant crown
Implant crown
 Implant bridge
Implant bridge
 Implant supported denture
Implant supported denture
Long-term Benefits of Implant-supported Tooth Replacement
- Restores natural biting and chewing capacity
- Virtually stops bone loss or deterioration
- Maintains integrity of facial structure
- Makes you look younger by restoring lip support and minimizing wrinkles
- Increases comfort
If you are considering dental implants, you must first ensure that you have healthy gums and adequate jaw bone. There must be sufficient bone to anchor the titanium implant firmly, leading to stability of the replacement tooth. This is crucial to the long-term success of a dental implant. Some people may require a bone graft prior to the implant placement if their bone is too thin or soft. Others may require a sinus lift for upper arch dental implants if there is not enough bone height in the upper jaw or the sinuses are too close to the jaw. To check your suitability for a dental implant, visit a trusted dental professional for a consultation. Factors such as jawbone height, density and depth can be determined by a cone-beam CT scan.
Implants are a safe and well-established treatment for replacement of missing teeth. Like natural teeth, dental implants will last for as long as you care for them. Hence you must commit to keeping the dental implants clean and healthy. Meticulous oral hygiene and regular dental visits are critical to the longevity of dental implants.
Make an Appointment
Frenectomy
What is a frenectomy?
A frenectomy is the removal or reduction in size of a band of tissue called a frenum.
Where is the frenum?
There are two frenums located in the mouth : the labial frenum and lingual frenum. The labial frenum is found in the upper arch, it is the tissue that connects the lips to the gums above the upper central incisors. The lingual frenum is located between the base of the tongue and the floor of the mouth.
When is a frenectomy needed?

Labial frenum Lingual frenum
Labial Frenectomy
When the upper frenum is too wide or long, it can create a space between the two front teeth. Patients undergoing orthodontic treatment (braces) may be advised to go through frenectomy to prevent the space opening between the upper front teeth. Labial frenectomy may also be advised for denture patients. When a denture wearer’s lips move, the frenum may be pulled against the denture, which can be painful and uncomfortable. Frenectomy is often performed to help dentures fit better.
Lingual Frenectomy (Frenectomy for Tongue-tie)
An unusually short or thick labial frenum can reduce the mobility of the tongue. This condition is commonly known as “tongue tie”. “Tongue tie” can lead to problems with tongue mobility, leading to difficulties with speech articulation and swallowing. Lingual frenectomy may be required to free the tongue.
What is the procedure like?
Depending on the patient’s condition, the frenum is removed or reduced in size with a scalpel (blade) or a soft tissue laser. In some cases, the dentist may use a combination of scalpel and laser to shape the tissue to get a desired outcome. Frenectomy is usually done under local anaesthesia although general anaesthesia can be considered for young children needing this treatment.
Make an Appointment
Sinus Lift
When is a sinus lift necessary?
A sinus lift is required if there is inadequate bone height in the upper jaw to support a dental implant. The maxillary sinus membrane is lifted upwards to create space for the additional bone. This may be needed if implants are indicated for the upper jaw.
A cone-beam CT (CBCT) is usually done for the assessment of the bone quality before planning for a sinus lift. This scan will allow the dentist to accurately measure the height, width, and density of your existing bone as well as to evaluate the health of your sinus, together with other considerations.
What happens during a sinus lift procedure?
Sinus lifts are usually performed under local anesthesia. The gum tissue will be raised to expose the deficient bone and the site prepared to receive the grafting material. A small window is opened in the upper jaw bone next to the sinus. The sinus membrane is gently pushed up and away from the jaw before the bone graft material is packed into space where the sinus was. Once the bone is in place, stitches are placed to hold the new bone material securely.
Your dentist will evaluate the surgical site and remove stitches 2 weeks after the sinus lift surgery. It will take several months for the bone material to harden and integrate with your jaw.
Make an Appointment
Wisdom Tooth Removal
Wisdom teeth, also known as third molars, typically appear between the ages of 16 and 25 years. If there is sufficient space for the wisdom teeth to erupt normally and be correctly positioned, they can be easily cleaned and therefore do not cause problems.

However, it is far more common for wisdom teeth to erupt partially, sideways, in the wrong direction or in a manner that makes it challenging to clean them properly. The pockets formed between the wisdom tooth and adjacent molar tooth creates a space where food gets trapped. These pockets cannot be reached by the toothbrush or dental floss, making them impossible to clean, leading to bacteria build-up and decay of the wisdom tooth or the adjacent molar. Sometimes, the adjacent molar may be so badly decayed that it needs root canal treatment to restore it. It may even need to be extracted if the tooth cannot be salvaged. Other risks include inflammation of the surrounding gum and infection. More serious complications such as cysts and tumours can also be caused by impacted wisdom teeth.
What are common wisdom tooth complications?
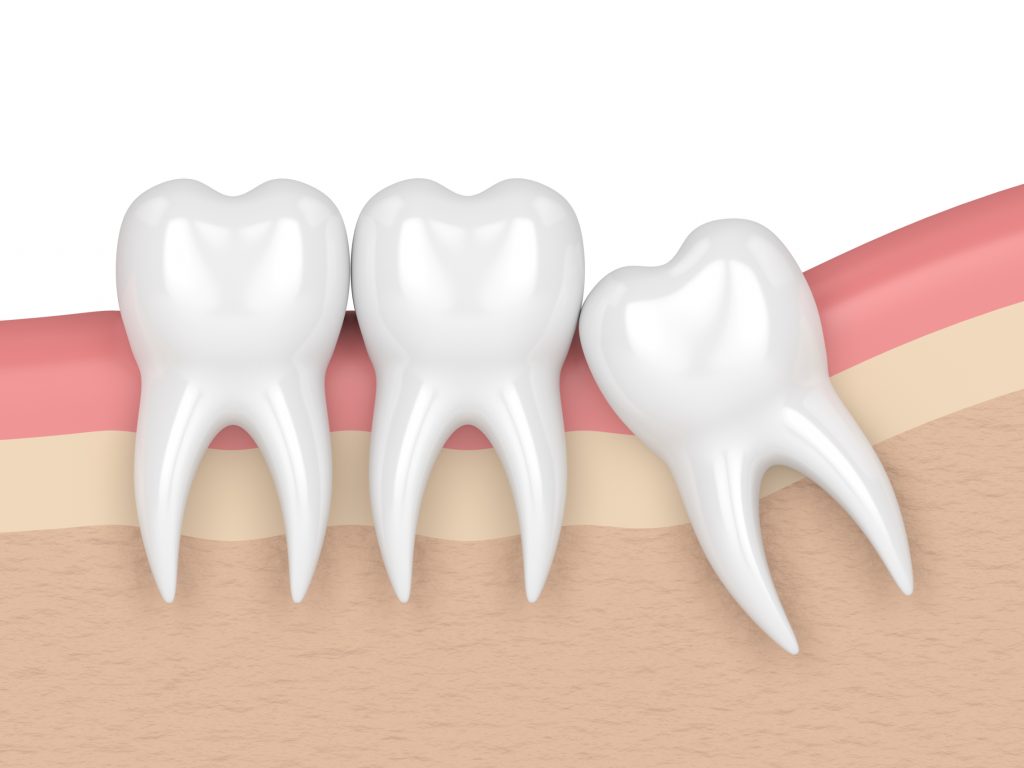 Mesial impaction
Mesial impaction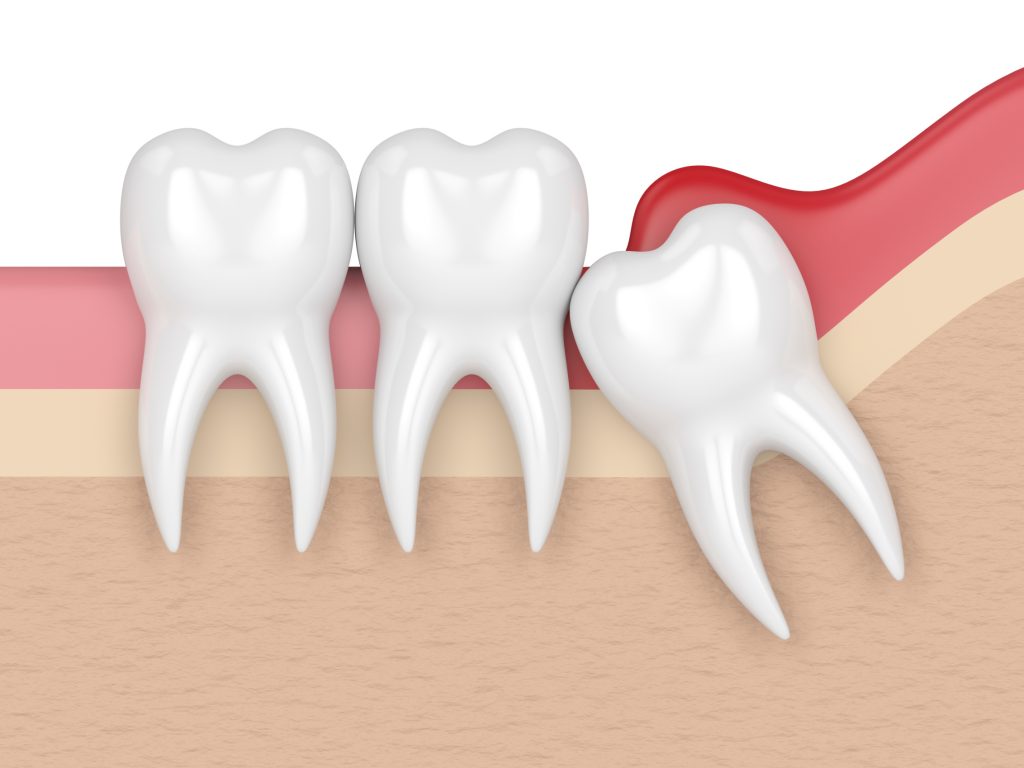 Mesial Impaction with Pericoronitis
Mesial Impaction with Pericoronitis
 Horizontal Impaction
Horizontal Impaction Distal Impaction
Distal Impaction
 Crowding of Teeth
Crowding of Teeth Erosion Cavity
Erosion Cavity
 Bone Cyst
Bone Cyst
What is the difference between wisdom tooth extraction and surgery?
Wisdom Tooth Extraction
A fully erupted wisdom tooth can be removed by wisdom tooth extraction, a procedure where the tooth is taken out after local anaesthesia has been administered to numb the area. This process is fairly straightforward.
Wisdom Tooth Surgery
An impacted wisdom tooth may partially emerge (partially impacted), showing only the crown of the tooth, or not emerge through the gums at all (fully impacted). The wisdom tooth may also grow at an angle towards or away from the second molar, or grow at a right angle, almost as if it is “lying” down.
For an impacted wisdom tooth, the removal process is more complicated as a surgical procedure is required to remove the tooth. The process would involve lifting the overlying gums to uncover the tooth and removing some surrounding bone in order to take out the tooth. Often, the tooth needs to be sectioned and removed in pieces. The gums are then sutured back in place. Wisdom tooth removal surgery is usually done under local anesthesia. It can also be done under sedation or general anesthesia if preferred.
What investigations are needed?
To determine the course of treatment for your wisdom tooth removal, a panoramic x-ray of your mouth is needed to check the wisdom teeth’s alignment and condition. The dentist will then advise you accordingly. In cases where the wisdom tooth lies close to the underlying nerve or other vital structures, a three–dimensional cone beam CT image may be required to plan for safe surgery.




 ENQUIRY
ENQUIRY